FDA Allows Pharmacists to Prescribe Paxlovid
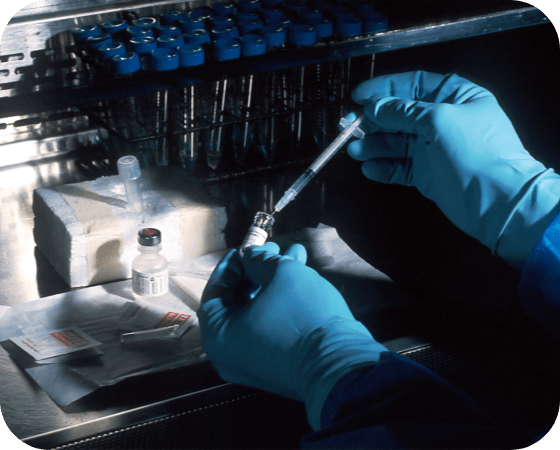
Authorized state-licensed pharmacists can now prescribe the COVID-19 antiviral Paxlovid to eligible patients, according to a revised emergency use authorization (EUA) from the Food and Drug Administration (FDA). The revision will increase access to the medication, which has been a priority of the Biden administration for the past few weeks. While Paxlovid has shown to be 89% effective in reducing the risk of hospitalization, use of the drug has been lower than expected due to complex eligibility requirements and reduced testing. The FDA has recommended that pharmacists refer patients for clinical evaluation if not enough information is available to assess possible drug interactions or renal and hepatic function.
BA.5 Becomes Dominant Omicron Subvariant in US
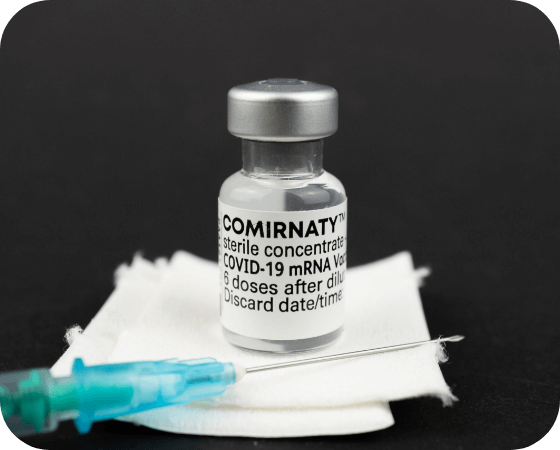
Omicron subvariant BA.5 comprises 53.6% of COVID-19 cases in the US, making it the nation’s dominant strain according to data from the Centers for Disease Control and Prevention (CDC). A similar subvariant, BA.4, makes up 17% of cases. Scientists estimate that BA.4 and BA.5 are about three times less sensitive to neutralizing antibodies from existing COVID-19 vaccines than the original Omicron subvariant BA.1, although current vaccines still offer strong protection against hospitalization and death from BA.4/5 infection. Due to waning vaccine protection, the FDA has recommended that vaccine manufacturers update their shots to specifically target BA.4/5 ahead of a fall booster campaign.
Senate Dems Release Updated Drug Pricing Proposal
On Wednesday, Senate Democrats released legislative text for an updated drug pricing proposal as part of an attempt to revive the reconciliation bill, Build Back Better that failed to move forward last year. While the text overall matches last year’s initial agreement, key changes include moving the implementation date for drug price negotiations from 2025 to 2026 and requiring Medicare to negotiate prices on as many drugs as possible in order to prevent future Republican administrations from interfering with negotiations. While there are no agreements on a broader reconciliation package, Senate Majority Leader Chuck Schumer (D-NY) has said that if a deal can be made, a bill could be considered on the Senate floor before August recess.
FDA Weighing Vin Gupta as New Advisor
According to reports, the FDA is considering tapping Dr. Vin Gupta, a pulmonologist and medical analyst for NBC, as a senior advisor to lead the agency’s communications strategy. The FDA’s decision to consider onboarding a communications expert is likely a response to the criticism over the agency’s messaging on baby formula and COVID-19 vaccines. Currently a chief medical officer at Amazon, Gupta his risen in prominence as a health commentator over the last two years of the COVID-19 pandemic and helped advise the Biden campaign and transition team on the pandemic response. If hired, Gupta would be responsible for reforming the FDA’s image as well as guiding the agency’s messaging on vaping and nicotine.
ICYMI: The Reflecting Pool Isn’t a Swimming Pool
Earlier this week, people were spotted taking a dip in the Reflecting Pool on the National Mall in Washington, DC, probably as a respite to the brutal humidity that’s been lingering around the region. Yesterday, the National Park Service erected a fence around most of the Reflecting Pool – seemingly as a way to keep swimmers out. This week’s escapades weren’t the first time people have used the Reflecting Pool for something other than its intended purpose – in 2018, some people took to ice skating on the pool during a particularly cold winter.